We are grateful to be able to share a deep and rich reflection from a now retired palliative care chaplain. Katie Herman worked at Abbott Northwestern Hospital in Minneapolis from 1996 to 2012 and as a member of its Palliative Care Team immediately after it formed in 2003. Then from 2012 to 2016, she participated in Allina Health’s Life Course in Late-Life Care. In this poignant and thought-provoking guest blog post, she talks a bit about palliative care, reflects on her experiences and approach as a chaplain, and shares some of her observations around end of life.
By Katie Herman
 “Death is not a medical event.
“Death is not a medical event.
It is a personal and family story
of profound choices,
of momentous words
and telling silences.”
~ Dr. Steven Miles, Professor Emeritus, University of Minnesota Center for Bioethics
One of the gifts of my life was to serve as a member of the Palliative Care Team at Abbott Northwestern Hospital in Minneapolis when it was formed in 2003—ultimately to become an inpatient and outpatient service that included physicians, advanced practice nurses, social workers, chaplains, and links to additional supportive and healing services. My desire to become a member of such a team was born in 1996, though at that point I had only heard the word “palliative” in connection with hospice—which was then most often still equated with “nothing more can be done.”
I now know that “palliative care” includes—but is not limited to—“hospice;” that it is an important support to patients and families as people seek treatment; and that it can, and often does, help people “do better longer.” I can also attest that neither palliative care nor hospice mean “nothing more can be done.”
Back to 1996—I can’t tell you the day or even the season, but I can tell you the encounter during which my passion for palliative care was ignited. I was visiting with a young woman whose mother had experienced a catastrophic brain hemorrhage and was being cared for in one of the Intensive Care Units (ICU) at Abbott. I had just been hired as ICU chaplain. Standing outside her mother’s room, this daughter tearfully told me, “This is hell—it is like watching an accident happen in slow motion, knowing your mother is on board, and knowing you can do nothing to stop it, and you can’t imagine she will survive. I don’t know what to do . . . ” Death is not a medical event but a personal and family story of profound choices, momentous words, telling silences.
Over the next four years, I would sit with many patients, but more often with family members, while superb medical and nursing care and precision technology and expertise sustained persons with life-limiting progressive or acute illness while the patient’s body tried to heal—or at least survive. In the midst of each ICU journey, patients and families often faced their mortality in a way they had not before. This was particularly evident when confronted with heart-rending decisions in which they felt like they were being asked to “play God.” Many families would say, “I just wish I knew what [my loved one] would say.”
In those days, I became a strong believer in advance directives. The guidance they can provide for the health care team, the suffering they can prevent for patient and family, and the assurance they can provide to loved ones sitting in those waiting rooms cannot be overstated. In those days, I also discovered that simply sharing the wisdom of my own mentor, Dr. Rachel Remen—often helped. Dr. Remen, co-founder and medical director of the Commonweal Cancer Help Program, in supporting people facing quandaries about treatment or care, counseled her patients to first ask themselves these three questions: Who am I? What is most important to me? How do I want to live?
 People’s reflections on these questions, or their loved ones’ reflections on their behalf, were so often rich in storytelling and indeed revealed what mattered most. And they also surfaced fears, sometimes burdensome regrets, and/or long-held but unrealized dreams.
People’s reflections on these questions, or their loved ones’ reflections on their behalf, were so often rich in storytelling and indeed revealed what mattered most. And they also surfaced fears, sometimes burdensome regrets, and/or long-held but unrealized dreams.
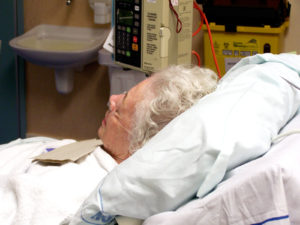
When asked what is most important to the patient, it was so often “family.” I was once paged to the ICU room of an elderly woman with dementia who was actively dying. When I got there, I was surprised to discover that she was sitting straight up in bed, delightfully chatting a mile a minute. I had to go check with her nurse to verify that I indeed had the right patient! When I returned, the woman was still talking, seemingly to anyone who would listen. Our conversation went something like this:
Her: “When I woke up this morning I was sound asleep!” [She laughed. So did I.] “I mean, when I woke up this morning, I thought, ‘I am supposed to be over there.’” [She was pointing out the window, describing wondrous scenes.]
Me: “Ohhhhh, you thought you were in heaven!”
Her: “Yes!”
Me: “Well this isn’t it! . . . But it seems that you might be going there soon. Is that okay with you?”
Her: “Oh yes.” [And she turned to look softly at her grieving husband to whom she had been married for more than 70 years.] “But you take care of him.”
She and her husband shared stories. We shared a prayer. When I left, they were chatting with the nurse. Within two hours, she had died.
Who am I? What is most important to me? How do I want to live?
Often I, along with colleagues and even families, would wonder: What if these conversations about what was most important, of meaning and hope (and fears) could happen much further “upstream” in the course of illness and loved ones’ life together? What if the person with a life-limiting illness had received support much earlier to have the conversations that matter with their families? What if they were aware earlier of the likely trajectory of their illness and the decisions that they might have to make—or that their loved ones would be asked to make?
Richard Groves, co-author of “The American Book of Living and Dying: Lessons in Healing Spiritual Pain,” identifies four areas of spiritual pain (and opportunity) people often experience near end of life. I found them to be recurring themes in my walk with those with life-limiting illness and their loved ones:

Meaning: Has my life mattered? Does it matter now? What have I done with my life? Is there meaning in what I’m going through now?
Forgiveness: This is a tricky one. Certainly, no one is perfect. All of us have things for which we carry guilt, shame, and/or remorse. Forgiveness cannot be mandated, and too many trauma survivors have been further wounded by such insistence from others. Still, my colleagues and I witnessed time and again how courage and grace have brought people to experiences of acceptance, forgiveness, and release, not only of others but of themselves too (sometimes the hardest task of all).
Relatedness: Among other things, this is the realm of grief inescapably at play as we move toward dying because it is the realm of loving and being loved (or our inability to do so). Whose am I? Where do I belong? Who will carry my stories? How do I even begin to say goodbye? Who am I within the web of life or the heart of the Divine
Hope: In the face of all the unknowns, what gives me hope? Into what or whom can I lean? Will my loved ones be okay? Do I have hope for the future of those I love? Do I have hope for the earth? What is next? In what can I trust?
Many have observed that end of life can be a time of great meaning and unexpected graces, and that people can heal even when a cure is not possible. I can attest to the healing that I was honored to witness time and again.
Who am I? What is most important to me? How do I want to live? As I slipped into my seventies this past August, I have found these questions have more and more guiding merit. But we don’t need to be at end of life—or even in our last chapter—to allow our reflections to clarify our values and to inform our living and our choices to love. I encourage us all to ponder these questions ourselves, to share them with those nearest to us. It matters.









